CUHK Study Finds Earlier Endoscopy Did Not Reduce Mortality and Risk of Further Bleeding in Acute Upper Gastrointestinal Bleeding Patients
The best timing for endoscopy of patients with acute upper gastrointestinal bleeding is still controversial among the medical community. A recent study conducted by the Faculty of Medicine at The Chinese University of Hong Kong (CU Medicine) found that for patients with overt signs of acute upper gastrointestinal bleeding, urgent endoscopy performed within 6 hours after gastroenterological consultation was not associated with lower mortality and risk of further bleeding, compared with endoscopy performed between 6 and 24 hours after consultation. In other words, earlier endoscopy did not lower mortality nor improve outcomes. The study results have just been published in the top medical journal, The New England Journal of Medicine (NEJM).
Aim at Finding the Best Timing for High-risk Patients to Undergo Endoscopy
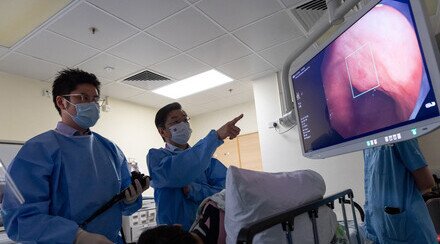
Acute upper gastrointestinal bleeding is one of the most common medical emergencies, common symptoms of which include hematemesis, melena, or both. Endoscopy allows healthcare professionals to identify the source of bleeding as well as haemostatic treatment for actively bleeding lesions, to reduce the risk of further bleeding and the need for surgery.
An international consensus group recommends endoscopy within 24 hours after presentation for patients with acute upper gastrointestinal bleeding. However, for patients who are at high risk of further bleeding or death, it has not been known whether earlier endoscopy would reduce the mortality rate.
The current study published in NEJM by the Institute of Digestive Disease at The Chinese University of Hong Kong aimed to find out the best timing for high-risk patients to undergo endoscopy.
Earlier Endoscopy Did Not Lower Mortality and Risk of Further Bleeding
From 2012 to 2018, the research team randomly divided 516 patients with high risk of further bleeding or death into two groups. These patients had overt signs of acute upper gastrointestinal bleeding and a Glasgow-Blatchford score of 12 or higher (scores range from 0 to 23, with higher scores indicating a higher risk of further bleeding or death). The two groups underwent endoscopy within 6 hours or between 6 and 24 hours after consultation, respectively. The results showed that in terms of 30-day mortality and percentage of further bleeding, there were no significant differences between the two groups.
| Urgent Endoscopy within 6 hr | Endoscopy after 6 hr but within 24 hr (N=258) |
|---|---|---|
Mortality at 30 days | 8.9% | 6.6% |
Further Bleeding within 30 days | 10.9% | 7.8% |
Duration of Hospitalisation (Median) | 5 days | 5 days |
The team also analysed the association between the time which patients underwent endoscopy and their risks of further bleeding and death. For patients who underwent urgent endoscopy within 6 hours during office hours (6:00 a.m. to 5:59 p.m.) and those whose endoscopy were performed after hours (6:00 p.m. to 5:59 a.m.), the percentage of further bleeding and death did not differ significantly.
Acid Suppression Before Endoscopy Reduces the Needs for Endoscopic Treatment
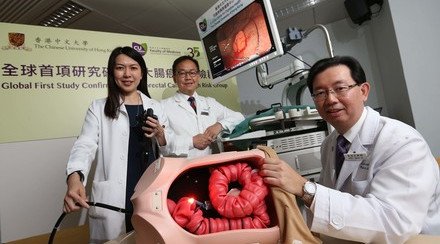
Professor James Yun Wong LAU, Chairman of the Department of Surgery and Yao Ling Sun Professor of Surgery at CU Medicine, remarked, “Urgent endoscopy with haemostatic treatment had been recommended by the medical community to patients with acute upper gastrointestinal bleeding. However, our study results showed that even if patients underwent endoscopy within 6 hours after gastroenterological consultation, their mortality rate, the incidence of further bleeding and duration of hospitalisation have not been reduced. The findings contrast sharply with our hypothesis that urgent endoscopy would be associated with improved treatment outcomes.”
Professor Lau continued, “On the other hand, patients who underwent endoscopy between 6 and 24 hours after gastroenterological consultation had waited for a longer period until endoscopy and received a longer period of acid suppression treatment. This reduced the number of ulcers with active bleeding. Thus, acid suppression before endoscopy can reduce the need for endoscopic treatment.”
The study results also showed that outcomes for endoscopy performed during office hours and those for endoscopy performed after hours were similar, suggesting that the quality of after-hours endoscopy was not inferior.
It is worth noting that this study excluded patients who had persistent hypotensive shock despite undergoing resuscitation and who required urgent endoscopy. The proportion of patients with variceal bleeding in the gastrointestinal tract in the study cohort was also small. Therefore, the findings may not be applicable to these groups of patients.
This research project is supported by the Health and Medical Research Fund of the Food and Health Bureau of the Government of Hong Kong Special Administrative Region.