CUHK Leads a Multinational Study that Finds New Treatment Paradigm of Mutated Lung Cancer
A multinational study led by the Faculty of Medicine of The Chinese University of Hong Kong (CUHK) has led to new treatment paradigm for epidermal growth factor receptor (EGFR) mutated lung cancer. For patients whose cancer genes further mutate and develop resistance after first-line EGFR targeted therapy, the new treatment can double the progression-free survival when compared with standard chemotherapy. Researchers of the study suggested that mutated lung cancer patients should be monitored in order to customize treatment approach targeted at the mutated genes. The findings have been published in the leading medical journal The New England Journal of Medicine, marking a new milestone for personalized medicine development of lung cancer. It is also an important breakthrough in lung cancer treatment which succeeded in providing a new line of defense on the battlefield against cancer.

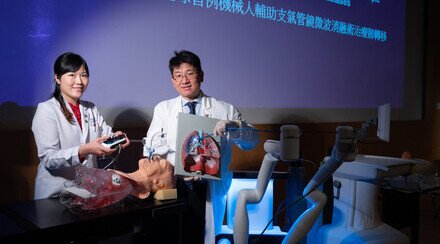
A multinational study led by Prof. Tony Shu Kam MOK, Li Shu Fan Medical Foundation Professor of Clinical Oncology and Chairman of the Department of Clinical Oncology of the Faculty of Medicine of CUHK (left), has led to new treatment paradigm for EGFR mutated lung cancer patients who develop resistance after first-line EGFR targeted therapy. The press conference is joined by Dr LAM Kwok Chi, Clinical Assistant Professor (Honorary), Department of Clinical Oncology, Faculty of Medicine at CUHK (middle) and a lung adenocarcinoma patient Ms. CHOW (right).
EGFR-mutated Patients Develop Resistance to First-line Targeted Therapy
Lung cancer is the most common cancer in the world, accounting for 1.6 million deaths every year. In Hong Kong, lung cancer is also the leading cause of cancer deaths and the second most common cancer with over 4,000 new cases per year. Lung adenocarcinoma accounts for about 70% of all lung cancers and many of the patients are female non-smokers.
EGFR tyrosine kinase inhibitor (TKI) is currently a first-line targeted therapy for lung adenocarcinoma patients with EGFR mutation. However, most patients treated with EGFR-TKI may develop resistance after 9 to 13 months of treatment and show disease progression. Standard chemotherapy becomes their only option. More than 50% of these patients are found to have T790M mutation.
Prof. Tony Shu Kam MOK, Li Shu Fan Medical Foundation Professor of Clinical Oncology and Chairman of the Department of Clinical Oncology of the Faculty of Medicine of CUHK, explained, ‘When EGFR mutation is being targeted by the therapeutic agent, cancer cells will “evolve” and a new driver oncogene will emerge. That’s why patients with EGFR mutation develop resistance to first-line targeted therapy.’ This process is called ‘cancer evolution’ and T790M mutation is one of the emerging driver oncogenes.
Prof. Tony MOK led a multinational study from 2014 to 2015 on 419 patients from around 20 countries with T790M mutations. All of them demonstrated disease progression after receiving first-line EGFR-TKI therapy. Patients were randomly divided into two groups; one group to receive a new molecular targeted therapy while the other with standard chemotherapy in the same period.
Results revealed that the new targeted therapy was more effective with a median of more than 10 months of progression-free survival, doubled that of standard chemotherapy (4 months). The response rate (i.e. percentage of patients with decrease in tumor size or disappearance of tumor in response to treatment) also doubled that of chemotherapy. It had fewer side effects and was associated with greater reduction in lung cancer symptoms.
| Molecular Targeted Therapy (279 patients) | Standard Chemotherapy (140 patients) | |
|---|---|---|
| Progression-free survival (Median) | 10 months | 4 months |
| Response rate (i.e. percentage of patients with decrease in tumor size or disappearance of tumor in response to treatment) | 71% | 31% |
New Treatment Paradigm of Mutated Lung Cancer
The findings were presented in the 17th World Conference on Lung Cancer organized by the International Association for the Study of Lung Cancer in Vienna in early December. Prof. Tony MOK said, ‘The significance of the study is that it transforms the practice of mutated lung cancer treatment. From now on, lung adenocarcinoma patients should not only undergo EGFR mutation test, but also need to be continuously monitored on how cancer “evolves” in their bodies. Once the disease progresses on first-line EGFR-TKI treatment, further mutation tests should be considered to customize the treatment.’
This remarkable research result by Professor MOK makes another important breakthrough in lung cancer treatment after his landmark study in 2009, which established the role of first-line treatment in patients with EGFR mutation, as well as his findings in 2014 proving that molecular targeted therapy is superior to standard first-line chemotherapy in ALK-positive lung cancer patients. By understanding the molecular profile of lung cancer, physicians could customize the treatment for patients according to the genetic information of their tumor. This brings personalized medicine development of lung cancer into a new stage and enhances patients’ quality of life.