CUHK dissects lung carcinoma at single-cell resolution uncovering a new mechanism for tumour formation
Tumour formation is a multistep and complex process and the underlying mechanism behind it is still largely unclear. A new study conducted by The Chinese University of Hong Kong’s (CUHK) Faculty of Medicine (CU Medicine) dissected the dynamics of lung cancer at single-cell resolution and successfully discovered a new mechanism for tumour formation via “macrophage-myofibroblast transition (MMT)”. Their preclinical work demonstrated its therapeutic implication for treating lung cancer in this first study to define a pathogenic role of MMT in cancer. The findings have been published in a high-impact international scientific journal Advanced Science.

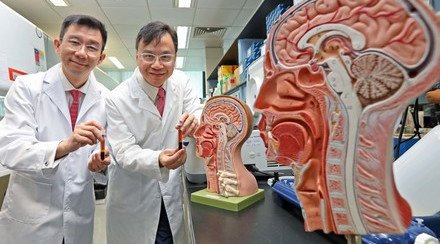
A new study conducted by CU Medicine dissected the dynamics of lung cancer at single-cell resolution and successfully discovered a new mechanism for tumour formation via “macrophage-myofibroblast transition (MMT)”. The finding may help design precise treatment plans for lung cancer. Members of the research team include (from left) Professor Patrick Ming Kuen TANG, Assistant Professor and Dr. Philip Chiu Tsun TANG, Postdoctoral Fellow from the Department of Anatomical and Cellular Pathology, Professor Hui Yao LAN, Choh-Ming Li Research Professor of Biomedical Sciences from the Department of Medicine and Therapeutics, and Professor Ka Fai TO, Chairman of the Department of Anatomical and Cellular Pathology at CU Medicine.
Better understanding of tumour microenvironment at single-cell resolution accelerates therapeutic development
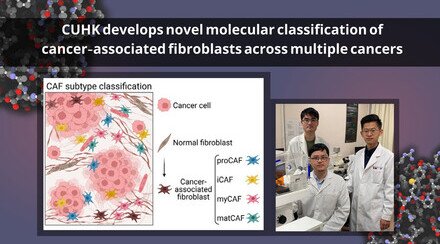
Cancer-associated fibroblasts (CAFs), the most abundant cell type in the tumour microenvironment, are important for tumour formation and progression including angiogenesis, immunosuppression, metastasis, and drug resistance. However, CAFs are highly heterogeneous and multifunctional and contain both “good” (anticancer) and “bad” (protumoral) subpopulations, making them difficult to target.
Single-cell RNA sequencing is an emerging technology to extract the genetic profile of every cell in a tissue sample with high precision. It serves as a perfect tool for the research team to capture the dynamics of the tumour microenvironment which may lead to the discovery of a new therapeutic strategy for targeting CAFs.
Professor Patrick Ming Kuen TANG, Assistant Professor from the Department of Anatomical and Cellular Pathology at CU Medicine said, “Single-cell RNA sequencing allows us to observe the dynamics of the tumour microenvironment in an unexplored dimension at the transcriptome level with single-cell resolution, and to distinguish between the “good” and “bad” cells which cannot easily be done by the conventional identification method with scalpel and microscope. It helps us to design precise treatment plans.”
First study to define a pathogenic role of “Macrophage-Myofibroblast Transition” in cancer
The mechanism by which immune cells, “macrophages”, are directly transformed into pathogenic myofibroblasts due to long-term overactivation is called MMT. This study further discovered that macrophages can also transform into protumoral CAFs in the tumour microenvironment via MMT for promoting tumour growth. The research team had previously discovered the association of MMT in kidney disease progression, and this is the first study to define a pathogenic role of MMT in cancer.
Dr. Philip Chiu Tsun TANG, Postdoctoral Fellow from the Department of Anatomical and Cellular Pathology at CU Medicine explained, “The advanced bioinformatics strategies pseudotime and RNA velocity allow us to capture the entire developmental process of the macrophages in lung cancer with the single-cell RNA sequencing dataset.” Dr. Tang has recently been awarded the UGC Postdoctoral Fellow Scheme 2021/22 and Young Investigator Award of the Hong Kong Society for Immunology 2021 for this discovery.
In addition, the team further identified a transcription factor Smad3 as the key regulator for initiating MMT in non-small-cell lung carcinoma by gene network analysis. They demonstrated that genetic or pharmaceutical inhibition of macrophage Smad3 effectively blocks MMT leading to tumour regression in mice, representing a potential therapeutic target for precisely eliminating the “bad” CAFs.
Professor Hui Yao LAN, Choh-Ming Li Research Professor of Biomedical Sciences from the Department of Medicine and Therapeutics at CU Medicine said, “MMT was discovered from renal fibrosis in 2014 and there are still a lot of possibilities for this novel mechanism in human diseases. Our next step is to develop its precision therapeutics for clinical use.”
Professor Ka Fai TO, Chairman of the Department of Anatomical and Cellular Pathology at CU Medicine added, “Although T-cell based immunotherapy performs well in leukaemia, less than 30% of lung cancer patients respond to it. A better understanding of the tumour microenvironment will improve the efficiency of immunotherapy for solid cancers, possibly by targeting the MMT.”

Findings have been published in high-impact international scientific journal Advanced Science.
This study was supported by the Hong Kong Research Grants Council, Faculty Innovation Award from CU Medicine, the State Key Laboratory of Translational Oncology, the Guangdong-Hong Kong-Macao-Joint Labs Programme from the Guangdong Science and Technology Department, and Lui Che Woo Institute of Innovative Medicine (CARE programme). Other main contributors to this study include Professor Alfred Sze-Lok CHENG, Professor Tin-Lap LEE, Professor Kam-Tong LEUNG, Professor Anna Chi-Man TSANG, and PhD student Jeff Yat-Fai CHUNG from CU Medicine. The original study can be accessed here: https://onlinelibrary.wiley.com/doi/10.1002/advs.202270005