CUHK Succeeded in Animal Study and Clinical Case of Percutaneous Nanoknife New Breakthrough in Cancer Treatment
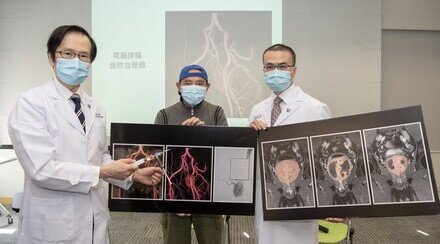
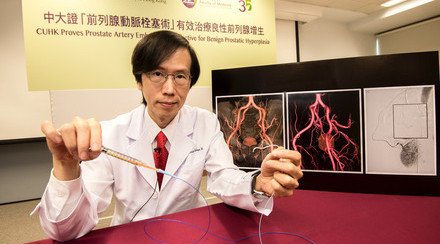
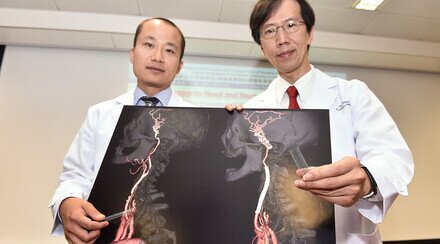
Prof. Simon Yu, Director of Vascular and Interventional Radiology Foundation Clinical Science Center and Professor of Department of Imaging and Interventional Radiology, The Chinese University of Hong Kong (CUHK) successfully completed a clinical case of percutaneous Nanoknife (Irreversible Electroporation) treatment on a liver cancer patient. The advantage of the treatment over thermal ablation techniques such as microwave or radiofrequency ablation is that it does not damage the blood vessels, bile ducts, or nerves near the tumors. It can be used to treat cancers in the liver, lung, prostate, head and neck, kidney, and pancreas without surgical operation.

Prof. Simon Yu, Director of Vascular and Interventional Radiology Foundation Clinical Science Center and Professor of Department of Imaging and Interventional Radiology, CUHK successfully conducted the animal study and clinical case of percutaneous Nanoknife.
Thermal ablation such as microwave ablation and radiofrequency ablation are widely accepted as effective treatments for liver cancer, with a clinical outcome comparable to that of surgical resection for liver tumor of size below 5cm. However, thermal ablation could not effectively eradicate cancer cells that are close to blood vessels due to the 'heat-sink' effect which prevents the building up of a tumoricidal temperature. As a result, recurrence of tumor in these areas tends to occur. Thermal ablation also causes thermal damage to bile ducts, gallbladder, and bowel, leading to bile duct occlusion, and perforation of gall bladder and the bowel. Nanoknife is a new technological breakthrough in cancer treatment, applicable to solid tumors of size less than 5cm and to tumors that are close to blood vessels, nerves and bile ducts.
Under the sponsorship of the Vascular and Interventional Radiology Foundation, Prof. Simon Yu and his research team successfully conducted an animal study on percutaneous Nanoknife between March and June of 2013. The objective of the animal study was to discover the short, middle and long term effect of Nanoknife on various organs of live pigs. It was revealed that Nanoknife is effective in causing apoptosis in the cells of lung, kidney and muscle; it does not cause damage to blood vessels, nerves, bile ducts, and bones; and it is not harmful to the stomach and urinary bladder when a safe distance is kept.
Building upon the favourable findings in the animal study, Professor Yu conducted a clinical study of percutaneous Nanoknife treatment on patients with liver tumor or pancreatic tumor of size less than 3cm. In November 2013, a clinical case of percutaneous Nanoknife treatment was successfully completed on a liver cancer patient. The patient was put under general anaesthesia using neuromuscular blockade to avoid skeletal muscle contraction. Under the guidance of ultrasound and CT, needle-like electrodes of 1mm diameter penetrated the skin to reach the tumor. Ultra-short but strong electric current was emitted by the electrodes in a controlled fashion to kill the tumor cells. The size and location of the electric field are calculated and mapped out electronically to ensure complete coverage of the tumor. The tumor cells are subsequently absorbed and replaced by normal healthy cells via the body's natural healing process.
Prof. Simon Yu remarked, 'Thanks to the generous support of the Vascular and Interventional Radiology Foundation, we completed the animal study in June 2013 and conducted the percutaneousNanoknife treatment in November 2013. The treatment lasted for just an hour and left only wounds of the size of needle holes on the patient's skin. The patient could be discharged on the next day after treatment. We shall continue our clinical trial and hope to introduce this new and effective treatment in local hospitals very soon.' (r).jpg)
(r).jpg)