CU Medicine Study Shows Childhood Obstructive Sleep Apnoea Increases the Risk of Hypertension in Adulthood

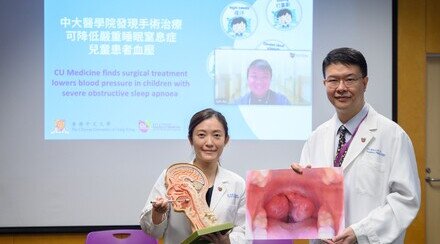
CU Medicine published the world’s first longitudinal 10-year follow-up study to evaluate the natural history and long-term impact of childhood obstructive sleep apnoea (OSA) on blood pressure outcomes in adulthood. Results showed compared to those who did not have OSA in childhood, children with moderate to severe OSA are 2.5 times more likely to get hypertension when they grow into young adulthood, increasing their risks of having cardio-cerebro-vascular diseases in the long run. (From right) Professor Albert Martin LI, Chairman; Dr. Kate Ching Ching CHAN, Clinical Professional Consultant and Dr. Jun Chun Ting AU, Research Assistant Professor of the Department of Paediatrics at CU Medicine.
Obstructive Sleep Apnoea (OSA) is a common sleep disorder that affects all ages, including young children. The Faculty of Medicine at The Chinese University of Hong Kong (CU Medicine) published the world’s first longitudinal 10-year follow-up study to evaluate the natural history and long-term impact of childhood OSA on blood pressure outcomes in adulthood. Results showed childhood OSA is an independent risk factor for higher blood pressure in adulthood. Compared to those who did not have OSA in childhood, children with moderate to severe OSA are 2.5 times more likely to get hypertension when they grow into young adulthood, increasing their risks of having cardio-cerebro-vascular diseases in the long run. The findings were published in world’s leading respiratory medicine journal Thorax.
5% of school-aged children in Hong Kong suffer from OSA
OSA is a common form of sleep-disordered breathing. It happens when the upper airway is obstructed during sleep, leading to pauses in breathing or hypopnoeas. The pause in breathing may occur many times in a night, disrupting the child’s sleep. In children, the most common cause for such a blockage is enlarged tonsils and adenoids. Untreated patients have higher risk of cardiovascular, metabolic or neurobehavioural complications. A previous CU Medicine study estimated about 5% of school-aged children in Hong Kong are affected by OSA.
Professor Albert Martin LI, Chairman of the Department of Paediatrics, CU Medicine elaborated, “OSA is common in children but often unrecognised. Snoring, night sweats and mouth breathing are some common symptoms of OSA. Other symptoms are daytime inattention, hyperactivity, sleepiness, and behavioural problems. It could be difficult for parents to associate these symptoms with sleep disorder, we therefore suggest to them that they seek medical advice if they find their children with these conditions. We also suggest that paediatricians routinely ask about OSA symptoms in their clinical practice.”
Dr. Jun Chun Ting AU, Research Assistant Professor of the Department of Paediatrics, CU Medicine said, “Blood pressure follows a circadian rhythm, with 10% to 15% lower values during sleep than during wakefulness. Previous studies have demonstrated that OSA patients, both children and adults, have higher blood pressure, especially during sleep, when compared to healthy individuals. Higher blood pressure during childhood precedes the development of hypertension in adulthood and will worsen cardiovascular prognosis. Therefore, their blood pressure has to be closely monitored in order to maintain good cardiac health, especially in children whom there will be a long-term effect.”

Professor Albert Martin LI says snoring, night sweats and mouth breathing are some common symptoms of OSA. Other symptoms are daytime inattention, hyperactivity, sleepiness, and behavioural problems. It might be difficult for parents to associate these symptoms with sleep disorder, he therefore suggests them to seek medical advice if they find their children with these conditions.

Dr. Jun AU says overnight polysomnography is a standard diagnostic tool for childhood OSA. It collects a range of physical data such as electroencephalography, electromyography and electrocardiography to evaluate the level of sleep obstruction.
CU Medicine was first to examine the effect of childhood OSA on adulthood blood pressure
CU Medicine’s Paediatrics Sleep Research Team conducted the world’s first longitudinal 10-year follow-up study to evaluate the natural history and long-term impact of childhood OSA on blood pressure outcomes. The team invited subjects from a cohort established between 2003 and 2005 for a childhood OSA epidemiological study to undergo overnight polysomnography and 24-hour blood pressure monitoring. A total of 243 participants attended the follow-up visit.
The mean age was 9.8 years at baseline and 20.2 years at follow-up, with a mean duration of 10.4 years. Below are the major findings:
Baseline status | Normal (98 individuals) | Primary snoring (49 individuals) | Mild OSA (75 individuals) | Moderate-to-severe OSA (21 individuals) |
Relative risk of having hypertension at follow-up (95% Confidence Interval) | Reference group | 1.9 (0.9 - 4.2) | 1.5 (0.7 - 3.0) | 2.5 (1.2 - 5.3) |
Dr. Kate Ching Ching CHAN, Clinical Professional Consultant of the Department of Paediatrics, CU Medicine said, “Our study showed childhood OSA is an independent risk factor for higher blood pressure in adulthood compared to those who did not have OSA in childhood. Children with moderate to severe OSA are 2.5 times more likely to get hypertension when they grow into young adulthood, which will increase their risks of having cardio-cerebro-vascular diseases in the long run. Diagnosis and early treatment of childhood OSA may help to reduce the healthcare burden related to cardio-cerebro-vascular diseases.”