CUHK-HKU collaborative study finds about 80% lower risk of death among COVID-19 inpatients prescribed oral medication and the risk of hospital admission in outpatients is significantly reduced by nearly 90%
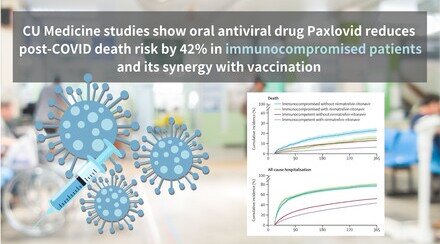
Two types of oral antiviral drugs have been prescribed to COVID-19 patients since the fifth wave of the pandemic in Hong Kong. A recent study led by researchers from The Chinese University of Hong Kong (CUHK)’s Faculty of Medicine (CU Medicine) and The University of Hong Kong’s LKS Faculty of Medicine (HKUMed) revealed that the oral antiviral agent strategy may reduce the risk of death in hospitalised patients by 76%. The risk of hospital admission in outpatients was also reduced by 88%.
Nirmatrelvir-Ritonavir (Pfizer’s oral drug) may save over HK$43,000 by preventing one death when compared to usual methods of care. The study findings have just been published in The Lancet Regional Health – Western Pacific.
Analysis of data on more than 50,000 COVID-19 patients from the fifth wave
The Jockey Club School of Public Health and Primary Care at CU Medicine and the Department of Emergency Medicine at HKUMed conducted a retrospective cohort analysis between February and March 2022, also known as the peak of the fifth wave, involving 54,355 COVID-19 outpatients in designated clinics and inpatients in public hospitals in Hong Kong. They evaluated the effectiveness of Molnupiravir (Merck Sharp & Dohme’s oral drug) and Nirmatrelvir-Ritonavir. The research included patients who were 60 years old or above, and patients under the age of 60 with at least one chronic disease. Among these patients, 20% were prescribed either one of the oral drugs.
The research team found that both Molnupiravir and Nirmatrelvir-Ritonavir were significantly associated with a reduced risk of death among inpatients. In hospitalised patients either Molnupiravir alone or Nirmatrelvir-Ritonavir prescription reduced all-cause mortality by 76%. Nirmatrelvir-Ritonavir reduced the risk of death by 90%, while Molnupiravir did so by 69%.
Among outpatients, prescription of Molnupiravir or Nirmatrelvir-Ritonavir lowered the risk of poor health outcome progression and unplanned hospital admissions within 28 days after attending outpatient clinics by 88%. Nirmatrelvir-Ritonavir reduced the odds for unplanned hospital admissions by 63% and Molnupiravir by 28%.
Among hospitalised patients, prescription of Molnupiravir or Nirmatrelvir-Ritonavir lowered the risk of unplanned hospital readmission within 28 days after admission to inpatient ward by 21%. Nirmatrelvir-Ritonavir had a significantly better reduction of 53% than Molnupiravir’s 29%.
Nirmatrelvir-Ritonavir saved over HK$43,000 to prevent one death, compared to usual methods of care
The research team also calculated the cost of preventing one death when compared to usual methods of care. In inpatient settings, Nirmatrelvir-Ritonavir saved HK$43,194 (US$5,503) to prevent one death, while Molnupiravir cost an extra HK$20,637 (US$2,629) to do so[1].
The research team pointed out that, although Nirmatrelvir-Ritonavir is more effective in reducing death risk and hospital admission, it has significant drug-drug interaction potential and may not be suitable for some patients who are taking blood thinners or antibiotics. The potential for Molnupiravir to interact with concomitant medications is considered low.
A triage mechanism may be worth considering for timely prescription of oral antiviral agents to COVID-19 patients with mild to moderate symptoms
Dr Crystal Chan Ying, co-first author of the study and Postdoctoral Fellow from The Jockey Club School of Public Health and Primary Care at CU Medicine, said, “In COVID-19 patients with mild symptoms, both Molnupiravir and Nirmatrelvir-Ritonavir prescriptions were associated with reduced all-cause mortality and healthcare utilisation, while Nirmatrelvir-Ritonavir was associated with significant cost savings in inpatient settings.”
Professor Eliza Wong Lai-yi, co-corresponding author of the study from The Jockey Club School of Public Health and Primary Care at CU Medicine, commented, “To ensure the sustainability of the healthcare system, it is recommended that a triage mechanism should be in place to refer COVID-19 patients with mild to moderate symptoms to designated clinics or collaborating general practitioners for timely prescription of oral antiviral agents.”
Importance of a real-world prescription data for timely prescription of oral antiviral agents to COVID-19 patients with mild to moderate symptoms
Co-first author of the study, Dr Abraham Wai Ka-chung, Clinical Assistant Professor from the HKUMed’s Department of Emergency Medicine and Consultant at The University of Hong Kong-Shenzhen Hospital (HKU-SZH), said, “This study examines the real-world prescription data about both Molnupiravir, Nirmatrelvir-Ritonavir and conservative management in wards, emergency departments and clinics. Timely treatment with these antiviral agents effectively protects our senior citizens and patients with chronic diseases infected with Omicron variant from hospitalisation and death. Our clinical and health economic analyses should inform the policy makers the direction of territory-wide infection management strategy.”
The other co-corresponding author, Professor Timothy Rainer from the HKUMed’s Department of Emergency Medicine, added, “This study deals with associations rather than cause and effect. Its findings suggest that these antivirals may save lives and costs but they need validation in clinical trials. In the absence of such trials, these data may cautiously and temporarily guide policy in the short term.”
[1] Cost-effectiveness of antivirals was estimated considering the 1) antiviral medication costs (Molnupiravir: USD306.40, Nirmatrelvir-ritonavir: USD205.94); 2) inpatient health care cost and the mean length-of-stay (Molnupiravir 9.97 days; Nirmatrelvir-ritonavir: 8.92 days) and 3) subsequent emergency department visit (Molnupiravir: reduce 29%; Nirmatrelvir-ritonavir: reduce 53%; average cost per ED visit: USD156.7).
Appendix
Table 1: Details of the study results
| Prescription of Molnupiravir or Nirmatrelvir-Ritonavir
| Prescription of Molnupiravir
| Prescription of Nirmatrelvir-Ritonavir
|
Reduction in the risk of death in inpatients | 76% | 69% | 90% |
Reduction of hospital admission within 28 days after attending outpatient clinics | 88%
| 28%
| 63%
|
Reduction of hospital re-admission within 28 days after admission to inpatient ward | 21% | 29% | 53% |
Healthcare cost per death adverted in comparison with usual methods of care | /
|
HK$20,637 extra |
HK$43,194 saved |