CUHK Introduces High Frequency Oscillations to Determine Resection Margin Increases the Effectiveness of Complex Epilepsy Surgery by around 30%
16 September 2015 A study conducted by the Faculty of Medicine at the Chinese University of Hong Kong (CUHK) reveals that in complex epilepsy surgery, combining intracranial electroencephalography (EEG) and high frequency oscillations (HFOs) technology can accurately determine the focal seizure origin and resection area, thereby increasing the surgical effectiveness by about 30%. The findings have been published in the Jan 2015 issue of the leading international journal Clinical Neurophysiology.

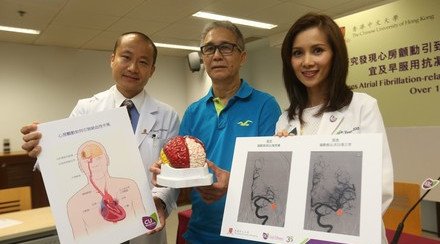
(From right) The CUHK medical team, including Dr. Chan Tat Ming, Clinical Associate Professor (honorary), Division of Neurosurgery, Department of Surgery; Prof. Poon Wai Sang, Head of Division of Neurosurgery, Department of Surgery; Dr. Leung Ho Wan, Clinical Associate Professor (honorary), Division of Neurology, Department of Medicine and Therapeutics; and Dr. Zhu Xian Lun, Clinical Associate Professor (honorary), Division of Neurosurgery, Department of Surgery, Faculty of Medicine, point out that the newly developed high frequency oscillations (HFOs) technology can accurately determine the focal origin of complex epilepsy cases, thereby increasing the surgical effectiveness by around 30%.
【Epilepsy】
Epilepsy is a common neurological disorder. Patients will have seizures or loss of consciousness resulting from intermittent abnormal excessive electrical discharge of nerve cells in the brain, which may lead to accidents. There are more than 70,000 patients suffering from epilepsy in Hong Kong. In other words, 1 out of 100 people has at least one seizure in his/her life. 30% of patients have recurrent seizures which cannot be controlled by medication. Their work and daily lives will be severely affected by frequent hospital admissions. For refractory cases, patients should consider undergoing resective surgery for the alleviation of seizures.
【Intracranial electroencephalography (EEG)】
One of the key factors for success in epilepsy surgery is finding the seizure origin. Patients may need to undergo a series of non-invasive tests before the operation, including video electroencephalography (EEG), magnetic resonance imaging (MRI), functional imaging, e.g. positron emission tomography (PET), and clinical psychology tests. The area of brain tissues for removal can be determined if findings from these non-invasive investigations are in agreement, pointing towards a focal seizure origin.
Prof. Poon Wai Sang, Head of Division of Neurosurgery, Department of Surgery at CUHK pointed out that MRI may not be able to show the diseased area in all cases. ‘Those cases without consistent results from non-invasive investigations will be defined as complex cases, which could not be treated through surgery in the past. It is estimated that there are around 3,000 patients in Hong Kong with epilepsy of such complexity. To help these patients, the Faculty of Medicine at CUHK introduced intracranial EEG monitoring in 2006. It involves an operation to place electrodes onto the brain surface or into the brain substance, where the electrodes record electrical signals directly from the brain. The signals will then be analyzed to locate the focal seizure origin.’
Dr. Zhu Xian Lun, Clinical Associate Professor (honorary), Division of Neurosurgery, Department of Surgery at CUHK stated, ‘From 2000 onwards, the Prince of Wales Hospital and the medical team of CUHK have performed 128 cases of resective epilepsy surgery. We have introduced intracranial EEG monitoring and the HFOs technology successively for complex epilepsy surgery cases, to provide a chance for patients who would not be offered any surgery without the new technique.
【Recent Development: High Frequency Oscillations】
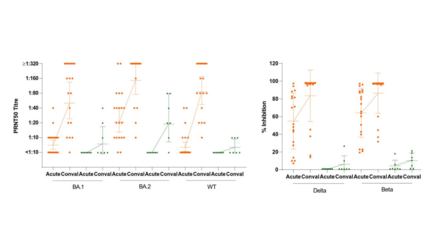
The medical team of the Faculty of Medicine at CUHK pioneered the use of combined intracranial EEG monitoring and the newly developed HFOs technology in 2012. The sophisticated method collects and analyses electrical signals between 80 and 500Hz at the beginning of a seizure. Findings indicated that it greatly increases the accuracy and effectiveness of complex epilepsy surgery. Up till now, the method has been applied to 7 patients suffering from epilepsy with high complexity. Operations have been carried out based on the investigation results, among which 71.4% achieved a good surgical outcome, which was an increase of 30% compared with 45.5% when the technology was not used.
Dr. Leung Ho Wan, Clinical Associate Professor (honorary), Division of Neurology, Department of Medicine and Therapeutics at CUHK explained, ‘Epilepsy surgery with high complexity has become possible since the introduction of intracranial EEG monitoring. First, a hypothesis will be formed based on non-invasive results. Then the electrodes will be implanted and the patient will be monitored in hospital for 1-2 weeks. The EEG signals are analyzed by experienced doctors and simultaneously collected for HFOs analyses. The new method provides obvious and clear data which enables the surgical team to precisely determine the focal seizure origin and resection area, thus increasing the surgical effectiveness.’
The research team is currently undertaking a larger study to investigate the application of HFOs technology.

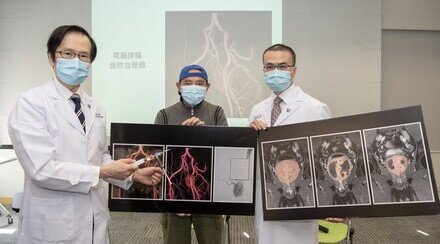
Mr. Au Yeung (left), who had suffered from complex epilepsy for 28 years, received intracranial electroencephalography (EEG) and high frequency oscillations (HFOs) monitoring in 2014. With the focal origin successfully located and resected, his frequency of incidence has dropped from around 20 to 4 seizures per year with much lighter symptoms.
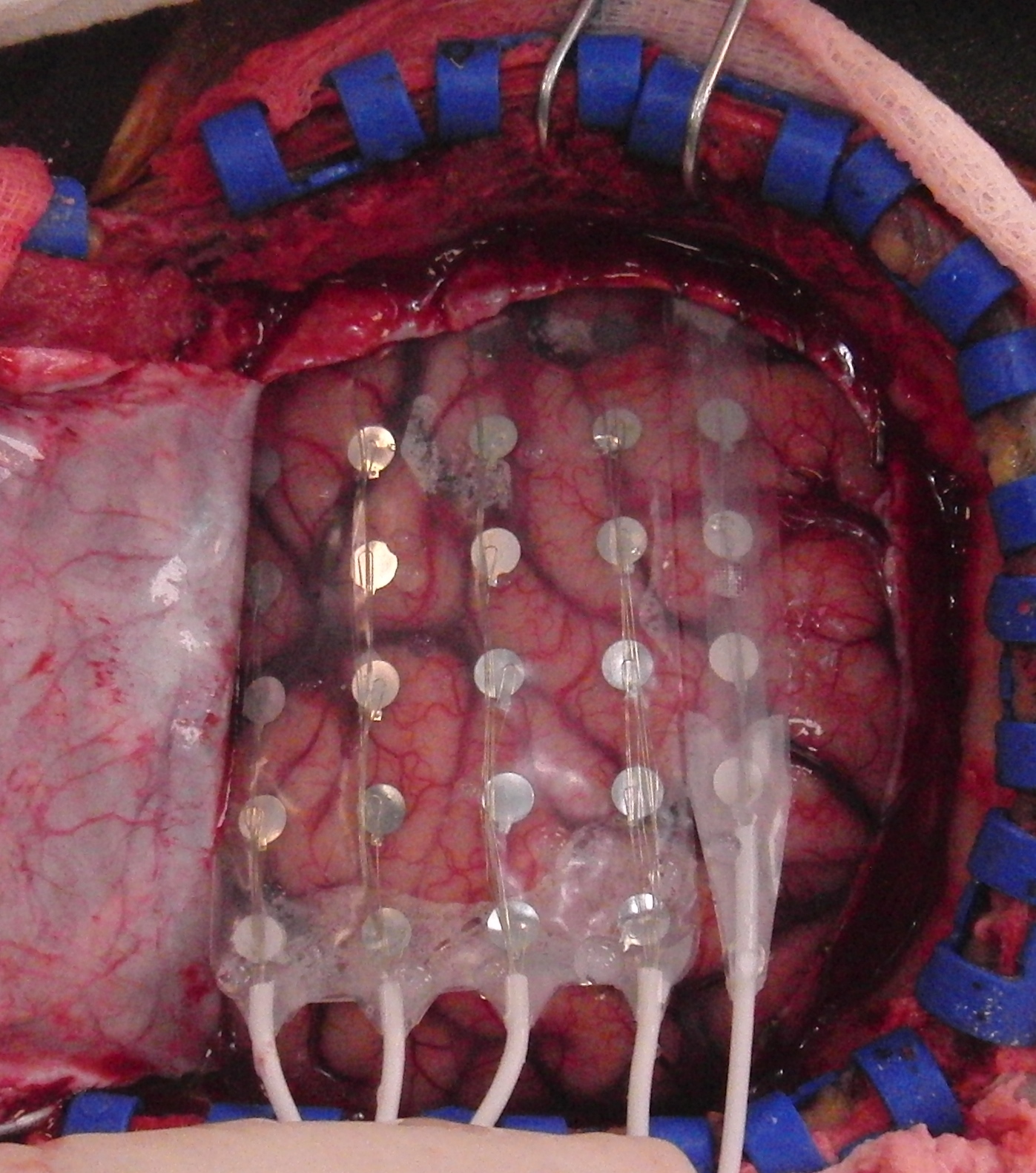
Those epilepsy cases without consistent results from non-invasive investigations will be defined as complex cases. Patients can consider undergoing an operation to place electrodes onto the brain surface or into the brain substance, where the electrodes record electrical signals directly from the brain. The signals will then be analyzed to accurately locate the focal seizure origin.